We have all heard it from our mothers or grandparents that how maintaining a proper lifestyle matters. But here is something most of us overlook: it matters just as much for your medication. The way your body responds to medicine can change depending on when you take it. So, I spoke to two doctors to dig deeper into how our circadian cycle affects drug effectiveness and what they think about modern medicine’s take on it.
That is what this piece is about. Read it to understand the science behind your body’s clock and why syncing with it could change how medicine works for you.
Table of Contents
What is Circadian Rhythm?
If you have ever watched cartoons, you have seen the classic scene: it is dawn, and the rooster crows, cock-a-doodle-doo! It’s not just for drama. It’s biology. As soon as sunlight hits its eyes, the rooster’s body kicks into gear. Turns out, we are not so different. Humans respond the same way. When light hits us, our body starts to function like clockwork. This is the circadian rhythm. The term comes from Latin: circa diem, meaning about a day. It’s how living organisms, including us, align their internal systems with the Earth’s rotation.
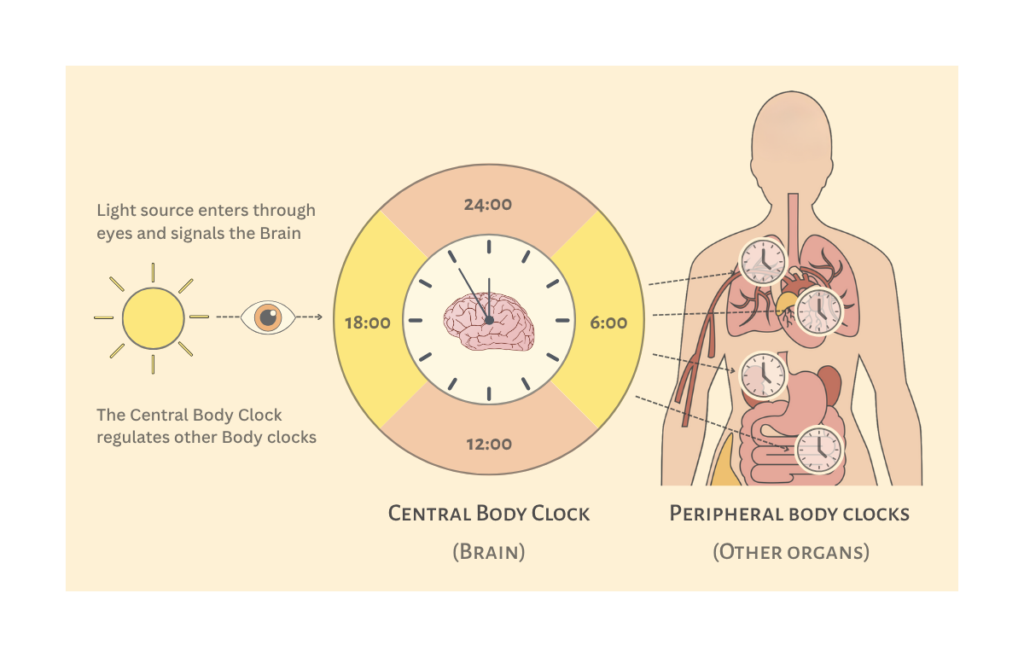
The body’s circadian system is wired to light. The moment sunlight enters through our eyes, it’s picked up by the brain’s- master clock, a tiny cluster of neurons that syncs our internal timing with the outside world. From there, signals ripple across the body, aligning everything with day and night. Each organ, each system, from digestion to the heart runs on its own rhythm, but they all take cues from this central clock. That is how our sleep-wake cycle, hormone levels (think melatonin and cortisol), body temperature, metabolism, and even cardiovascular activity stay in check. But in today’s fast-paced life, a bigger question comes up: why does timing matter so much to the body? And this takes us to our next section.
Why Timing Matters When Taking Medicines
When you take your medicine is just as important as what you take. There are two key ways to look at it:
- When the disease is most active
- And when it is at its weakest
Both are crucial for effective treatment.
Let’s start with infections. Whether it is bacteria or a virus, your body’s immune system does not work the same round the clock. It is most active during the day and interestingly, so are the invaders. Microbes like bacteria and viruses follow their own circadian rhythms. Many are weaker during the day. That is why daytime medication can be more effective: your body and the drug are fighting in sync.
It also explains something familiar, you feel mostly fine during the day, but when you wake up after a viral infection, bam- fever, body ache, runny nose. Now you know why: your immune system slows down at night, giving the virus an edge.
Another clear example? High cholesterol.
Cholesterol is produced throughout the day, but levels peak at night. That is why doctors often prescribe cholesterol-lowering drugs (like statins) to be taken at bedtime, so they can target the surge.
In diabetes, it is about insulin sensitivity. Your body responds better to insulin in the morning, and the effect tapers by evening. That is why the timing of antidiabetic medication matters, though it also depends on the type. Some drugs, like metformin, are taken after meals. Others, like sulfonylureas, are taken before.
Blood pressure follows a rhythm too. It rises sharply in the morning, that is when most heart attacks and strokes happen. Taking BP medication at night helps blunt that early-morning spike, offering protection when you need it most.
The takeaway?
Diseases and drugs do not just work in isolation they operate on a schedule. Syncing your medication with your body’s internal clock is not just smart. It’s science.
Also Read: Taking Supplements Without a Doctor? Why It Could Be Risky And What to Do Instead
Do Doctors Follow Chronopharmacology?
I spoke to two doctors. One had limited knowledge of timing-based treatment. The other was not aware of it at all. Turns out, this is not rare. A published study from a major hospital treating complex cases found something similar: only a handful of doctors understood or used the concept of chronopharmacology in practice. The doctors I interviewed reflected that same pattern.
“A doctor should study the pharmacodynamics and pharmacokinetics of a medicine before prescribing it. But this is where the education system falls short. We learn about these things in second year under a pharmacology professor — but by final year, it all fades.”- Dr. HBK Gantayat
Medicines That Require Chronopharmacological Consideration
Because most doctors are not formally trained in chronopharmacology, many prescriptions miss the timing factor entirely. But for some medicines, when you take them is just as critical as what you are taking.
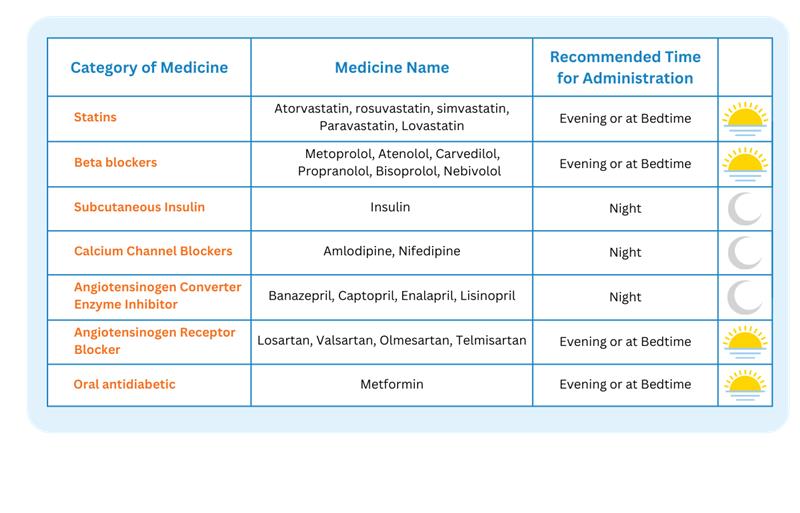
Here is a breakdown of drug categories where timing matters, and what the optimal window looks like:
Also Read: What is Really Inside Your Medicine?
Conclusion
Modern medicine has made massive leaps in what doctors prescribe. But it is still catching up on when to prescribe. Chronopharmacology is the science of timing medications with our body’s rhythms, is not a hypothesis. It is biology. And it is backed by data. Yet, as we have seen, awareness remains low. Medical education only touches the basics. Most prescriptions still follow a one-size-fits-all approach, ignoring the body’s natural timing.
The good news? We can change that.
Better awareness, smarter prescribing, and a deeper respect for our circadian rhythm can make medicine work with the body, not just inside it. Because the next big breakthrough in healthcare may not be a new drug – it may simply be better timing.
Mahak Phartyal completed her bachelor’s in pharmacy from Veer Madho Singh Bhandari Uttarakhand Technical University. She previously worked as a Medical Writer at Meril Life Sciences, where she wrote numerous scientific abstracts for conferences such as India Live 2024 and the European Society of Cardiology (ESC). During her college years, she developed a keen research interest and published an article titled “Preliminary Phytochemical Screening, Physicochemical and Fluorescence Analysis of Nyctanthes arbor-tristis and Syzygium cumini Leaves.”












I love it when people come together and share opinions, great blog, keep it up.